A woman spends her night sitting in a hospital chair. She sleeps in fits and starts, her body aching with exhaustion. In just a few weeks, she learned to arrange pillows, decipher the language of the monitors, and insist on medications that are usually unavailable.
She gets up every time her mother—or her husband, or her sister, or her son—opens her eyes, as if she could protect her from fear by hiding her own. From her bed, she watches her. She notices the dark circles under her eyes, overhears conversations about debt, understands that the illness no longer just affects her body: it has begun to devour the lives of her entire family… and then she utters the phrase no one wants to hear:
“I don’t want to be a burden anymore.”
Last November, a citizen initiative to legalize euthanasia in Mexico was presented to Congress. The project, known as the Transcendence Law, would allow people with a terminal illness or a debilitating chronic-degenerative disease or condition to request medical assistance in dying, provided they meet capacity requirements, have two medical diagnoses, and express their wishes freely, in an informed and repeated manner, and in writing, before a Notary Public… yes, before a Notary Public.
The initiative is presented as the legal recognition of autonomy in the face of pain, allowing people to make conscious and free decisions about their own lives, as a respect for human dignity and as universal access to healthcare, since it guarantees that this “right” can be accessible and real for everyone.
But there is a question that the enthusiasm for autonomy, dignity, and universal access to healthcare relegates to the background: what does it mean to choose when the real options for living without pain or with sufficient support are profoundly unequal in our country? Mexico is a nation where palliative care is not equitable, where home care is limited, and where the daily responsibility for care effectively falls on families. They are the ones who absorb the economic, physical, and emotional costs of prolonged illness. They pay with dwindling savings, abandoned jobs, and suspended life trajectories.
There are no support networks, nor are there consolidated public or labor policies that allow caregivers to provide care without falling into precarious situations. In most cases, staying alive means dragging the entire family into exhaustion.
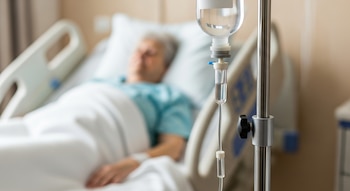
A person lies in a hospital bed receiving intravenous treatment, reflecting the importance of specialized medical care for critically ill patients. The image highlights the hospital environment and the resources needed to provide adequate care. (Illustrative Image Infobae)
And that fact radically alters the meaning of the discussion…
Because the patient looks around: they see the daughter who quit her job, the family conflicts, the husband who can’t sleep, the grandchildren who are waiting, and the family that is holding on as best they can. They perceive the immense effort of each day, and in that atmosphere, the desire to die can become intertwined with the desire to free others. It doesn’t arise solely from physical pain, but also from guilt, love, and the fear of continuing to demand sacrifices.
That is not full autonomy. It is autonomy wounded by inequality.
That is why the discussion opened by the Transcendence Law must include a prior question: what real support do we offer the patient to continue? How many requests would there be if families weren’t exhausted? If there were constant professional help, guaranteed rest, financial support, and emotional accompaniment? Probably fewer… perhaps far fewer. And the meaning of the debate lies in that difference.
It is contradictory to present euthanasia as part of the right to healthcare when the healthcare system itself is incapable of guaranteeing, with the same strength, timely treatment, effective pain relief, continuous support, and genuine assistance to patients and their caregivers. The option of ending life is offered as a service, while the right to healthcare remains largely dependent on the private efforts of families. The State would facilitate the procedure for dying, but it has not yet ensured the conditions for caring for those suffering from the illness and their caregivers.
Source: infobae




